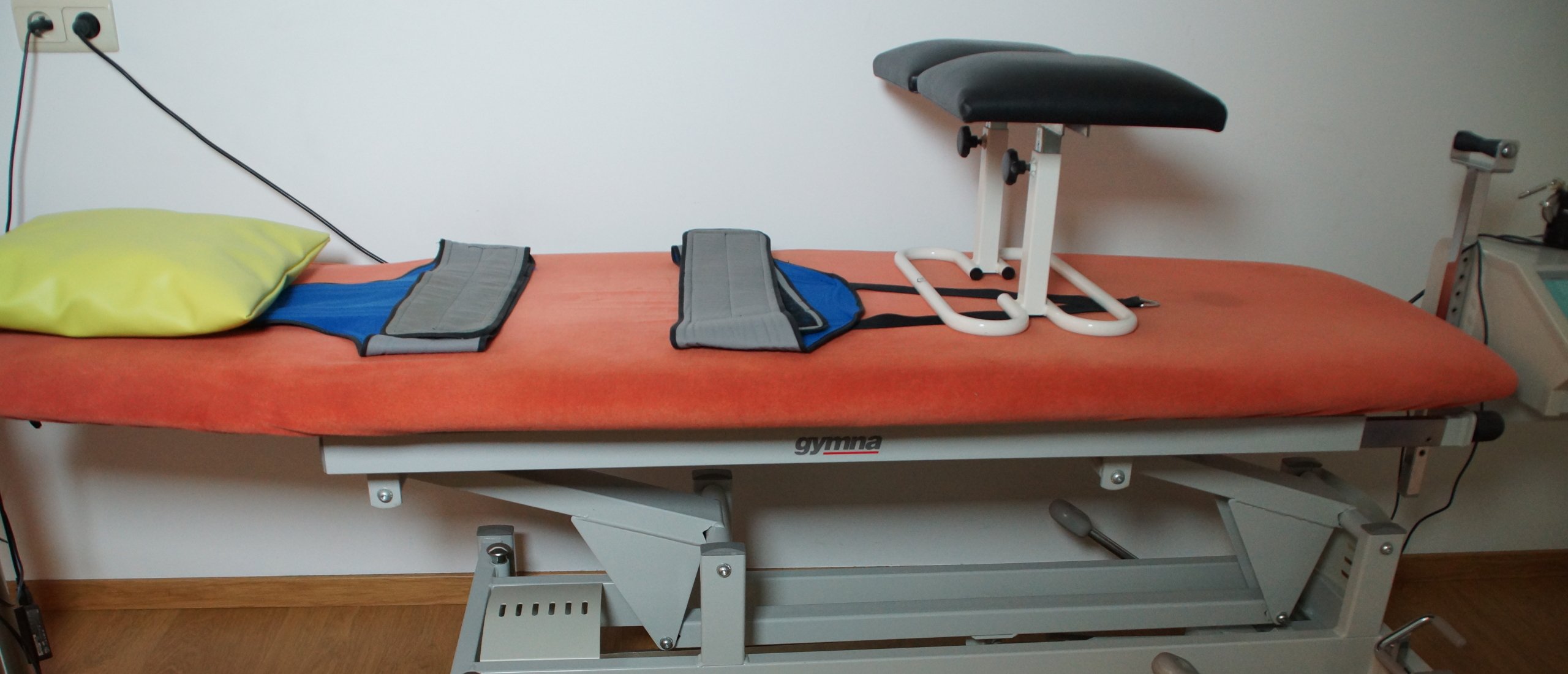
When to apply mechanical traction in the lumbar spine?
Mechanical traction for lumbar spine internal derangement?
Applying mechanical traction in the lumbar spine in order to reduce an internal derangement, is it an illusion or not?
It al depends on the clinical image of the patient: not every patient suffering from an internal derangement will react well on lumbar mechanical traction.
This is an interesting treatment method for a specific sub-group of lumbar patients. Several elements from the history and the functional examination will help us to determine whether or not a patient is more suitable for mechanical traction.
Discover here when and how to do it.
In this webinar recording you will find out all the details.
Patient selection is an important key factor which has an impact on your treatment results. Objective clinical reasoning and careful interpretation of the clinical examination procedure is therefore crucial. You would like to find out more? Why don't you join the Mastermind private training in orthopaedic medicine?
Effects of lumbar mechanical traction
Reduction of a disc protrusion by traction was first suggested by Dr. Cyriax in 1950. In the meantime this procedure has been optimized.
Sustained traction has three effects on the lumbar spine.
- The distance between the vertebral bodies increases, which creates more space for reduction.
- The posterior longitudinal ligament tautens and thus exerts a centripetal force on the protrusion. As a consequence a posterocentral protrusion responds better to traction than a posterolateral or lateral protrusion.
- Discography shows that a subatmospheric pressure is induced, by which a centripetal force is exerted upon the protrusion. Reduction of herniated bulges has been demonstrated on epidurography and CT scan during and after traction.
The effect depends on the force applied, the length of time, the interval between sessions and the total number of sessions. It is also an illusion to think that every internal derangement or protrusion can be reduced by traction. Similar to the manipulation strategy discussed higher, we are going to decide to apply mechanical traction or not, base don elements from the history and the clinical examination.Indications
Sustained mechanical traction can be considered in the following disorders : - A lumbar nuclear disc protrusion
- A mixed protrusion (partly annular, partly nuclear)
- S4-pain : only a very cautious attempt. In case of incontinence the patient should be referred at once o An upper lumbar disc protrusion (L1 and L2)
- A recurrent disc protrusion at the same level after laminectomy
- A primary posterolateral protrusion which lasted less than three months.
Contraindications
- Acute lumbago (annular or nuclear) o each movement causes twinges in the back and/or the lower limb. This is THE contraindication. The patient could be comfortable during the traction, but when the tension is released, the patient is much worse. It may take one hour or more before he can get off the table. This should be avoided
- An annular protrusion --> manipulation is a better idea
- Patients over +/- 65 years of age --> the water content of the disc has largely receded at that age. Applying traction or not in similar cases is a subjective manner, depending on the information from the history
- Certain cases of sciatica o with neurological deficit (sensory and/or motor)
- with gross lateral or flexion deviation
- sciatica which has persisted for six months in a patient under 60y (i.e. over ½ of the spontaneous evolution)
- Primary posterolateral protrusion of over three months’ standing
- Pregnancy o from the fourth month onwards
- Respiratory or cardiac insufficiency o the patient does not tolerate the thoracic harness. A patient with a cold should not be put on traction, because a cough or a sneeze during traction can be very painful. (The same applies for laughing !)
- Immediately after a manipulation session
- Any situation in which traction cannot be given comfortably
- Some patients experience a kind of claustrophobic feeling under traction
Practical aspects of lumbar traction
➔ Position of the patient / criteria - Traction can be given in several positions. The more common one is with the patient supine, using a pelvic and a thoracic harness with the straps anteriorly.
- If the patient is more comfortable in flexion and extension in standing is limited and painful, a flexion bench under the patient’s knees is used
- If extension is comfortable and flexion is the main problem, we put small cushions under the knee (and perhaps a small cushion can support the lumbar spine). Positions in prone lying are described in literature, which in theory are useful ; in practice, however, they are less feasible.
➔ Traction : intermittent or not ? Force ?
In order to reduce a disc protrusion constant traction is preferred ; most references show that intermittent traction is not efficient to reduce a lumbar disc protrusion. There is increased motor activity of the sacrospinal muscles on an EMG during traction, until the mechanoreceptors in the tendons are stimulated. From that moment, motor activity is inhibited, the intervertebral joint takes the strain and the reduction of the pulpy mass starts slowly. EMG silence is reached after 3 minutes. This suggests that traction must be sustained. At least 30-35kg traction force is required to influence the lumbar spine. A traction force of 25% of the body weight suffices to get a vertebral separation, but we need a traction force which is strong enough to reduce a protrusion.
The first session we give about 36 kg of traction for about 20 minutes. In the next sessions, duration and amount of traction increase. Mostly we don’t give more than 50-55 kg (depending on the morphology of the patient) for about 35 minutes.
➔ After the traction
The tension should be released very gradually, without any abrupt movement : choose the lowest possible release speed on your traction apparatus. Then the harnesses are opened, the thoracic one first. This too should be done smoothly, to avoid painful twinges. After traction the patient should not stand up straight away ; the transition from e.g. -45kg to +65kg needs to happen slowly in order to avoid pain.
The patient performs some gentle movements in supine lying : flexing and extending a knee, with both knees together small pelvic rotations, and eventually lifting his pelvis off the couch. If he manages all this without any discomfort, he can now get off the couch : rolling on to one side, bending both knees, bringing both feet outside the couch, pushing himself up into sitting, and standing up immediately. For the next ten minutes or so, sitting should not be allowed : he goes for a little walk before driving home. He should drive as little as possible and only with a cushion behind the back ; he should also avoid sitting as much as possible. Cave : first flexion could be painful
Traction Strategy
Results:
Treatment is given 5x/week if possible Two to maximum three weeks are required. Before each session the patient is examined, in order to assess the evolution. We expect improvement to start after a couple of days ;
if not, reassess and perhaps change the position in which traction is given. If there is no improvement after one week, traction is abandoned and another strategy is called for. If the symptoms are much better after two weeks, but have not disappeared completely, a third week’s treatment follows.
So, we give a maximum of 15 sessions. A CT-scan study shows reduction of disc material taking place in 78,5 % of central, in 66,6 % of posterolateral and in 57,1 % of lateral protrusions. This is biomechanically logical, since the presence of the (narrow) posterior longitudinal ligament (low lumbar segment) fascilitates the reduction of central protrusions, but has no extra effect on lateral protrusions.
