Shoulder non-capsular pattern, the diagnostic options
Acute subdeltoid bursitis
The acute bursitis is totally different pathology than the chronic one. The clinical difference between both is discussed in another article.
The onset is rather spontaneous. The disorder occurs at any age from adolescence onwards. It becomes much rarer only after the age of 65.
The entire bursa (subdeltoid AND subacromial part) is inflamed.
The patient has a very severe arm pain along the C5-dermatome. Spontaneous recovery takes about 6 weeks ; the pain is really severe and constant in the first 7-10 days.
Typical history
Spontaneous onset of slight arm pain the first day and some discomfort on elevation, much worse the next day with more difficulty in moving the arm ; the third day, the patient can hardly elevate the arm (maybe just some 30°) because of acute constant pain.
Examination : a clear non-capsular pattern.
- A elevation very painful and limited
- P elevation very painful and limited,muscle spasm end feel
- P rotations painful and less limited, muscle spasm end feel
- Probably also pain om some resisted tests (e.g. abduction, lateral rotation)
- Tenderness on palpation along the subdeltoid part of the bursa
Treatment
If the patient is seen within the first week, a strong analgesic injection followed by two infiltrations of triamcinolone in the entire bursa (subdeltoid and subacromial parts). As from the next day, the patient is 80 % better ; if needed, another infiltration is given a couple of days later.
Some taping can be used in order the decrease the subacromial compression and to reduce the compression on the bursa.
Controversy ?
The clinical image of an acute bursitis may be similar to the one of an acute calcific tendinitis (usually supraspinatus). The calcific deposit increases in size and ruptures into the subdeltoid bursa. MRI scan would confirm the presence of calcific deposits and/or inflammation in the subacromial space or overlying rotator cuff.
“Psychogenic” limitation
Psychogenic patients can show a rather particular pattern :
we need to compare the range of passive glenohumeral abduction with that of passive elevation (I refer to the chapter on shoulder functional examination). The passive abduction is a shoulder joint test (normal range of motion 90°), the passive elevation is a shoulder girdle test.
Even without glenohumeral abduction, there should be at least 60° of elevation, because of the activity of the serratus anterior who is responsible for the scapular rotation.
The elevation range of motion, therefore, should always be greater than the glenohumeral abduction range of motion. The patient is not aware of this clinical difference.
Psychogenic patients almost never say that a certain test does not hurt ; mostly, on each test, they describe some very vague undefined symtoms. The never clearly say “yes” or “no” when asked “does that change anything”.
Contracture after radical mastectomy
A painless scar, resulting in a limitation of passive elevation, whereas the passive glenohumeral abduction is normal.
Pulmonary neoplasm
A tumour in the base of the lung compressing the diaphragm. The diaphragm is a C4-
structure, hence there will be reference of pain in the C4-dermatome.
When this tumour invades the lower ribs, these will not tolerate any further stretching on elevation. Consequently, a spasm of the pectoralis major muscle is seen on any attempt of raising the arm above the horizontal, resulting in a limitation of elevation.
Contracture of the costocoracoid fascia
This minor disorder is very rare, sometimes congenital. It is somewhat more frequent after abdominal or thoracic surgery. The patient experiences some pectoro-scapular pain in an extreme positions. On examination, there is a slight limitation of scapular and arm elevation.
Acromioclavicular joint sprain
Could be the result of a traumatic lesion (fall on the shoulder with the arm at the side (fooball, hockey, skiing, judo,…)) or osteoarthrosis.
Clinical image
- Pain in the C4-dermatome
- End range pain on passive elevation and passive rotations
- Most positive test will be the passive horizontal adduction
- Possibly the resisted adduction might be slightly painful too
- If the upper part of the AC-joint is lesioned then there is tenderness on palpation
- If the lower part is lesioned we will also find a positive painful arc on elevation in the functional examination.
If the lesion is confined to the upper part, then DTM can be given. For the deeper part infiltration is the treatment of choice.
Anterior capsular contracture
The patient had an injury (not necessarily a dislocation) long time ago ; perhaps at that time he was even too young to develop a traumatic arthritis (which we normally don’t see under the age of 40 years).
The lesion remains localized and a capsular contracture supervenes.
On examination, we find that some lateral rotation is lost (about -20°) and that the end-feel has hardened.
Similar capsular contracture may occur 5-6 months after a complete rupture of the infraspinatus tendon : the small teres minor muscle cannot compete properly against the four strong medial rotators, hence the end of range in lateral rotation is not reached any more and part of the movement goes lost.
Subcoracoid bursitis
In that case the passive lateral rotation will also be limited and painful.
The movement is limited because of pain : the structures which are stretched on passive lateral rotation exert pressure on the inflamed bursa.
The treatment is an infiltration of triamcinolone.
How can we differentiate between the two disorders ?
Anterior capsular adhesions | Subcoracoid bursitis |
Trauma long time ago | Possibly spontaneous onset or overuse |
P lateral rotation limited harder end feel | Elastic end feel |
P lateral rotation performed from 90° abduction is also limited | Less limited when executed from 90° abduction |
Palpation negative | Palpation positive |
Mononeuritis
A mononeuritis has a typical clinical image :
- Constant pain for some 3 weeks
--> Pain is independent from movements, activities or positions - Pain in the scapular, suprascapular and upper arm area
- Muscular weakness for some months (4-8 months)
Cause ?
- Unknown
- Trauma ; traction injury to the nerve
- After fascial surgery
- Viral infection
Long thoracic neuritis
Limitation of active elevation is the problem. Passive elevation is not limited.
As described before, 180° of elevation consist of three components : 90° glenohumeral abduction + 60° scapular rotation + 30° glenohumeral adduction .
In that case the 60° of scapular rotation are at fault. This movement is mainly performed by the serratus anterior muscle, with the help of the trapezius muscle.
Since the long thoracic nerve innervates the serratus anterior, there will be weakness of this muscle resulting in about -45° limitation of ROM of active elevation.
Complementary test in case of a long thoracic neuritis: leaning forward with outstretched arms against a wall, which would show a scapula alata on one side.
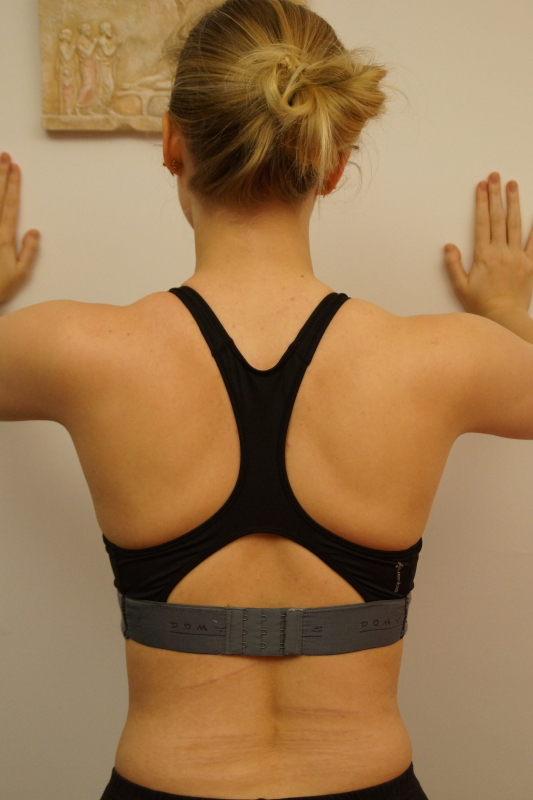 Scapula allata test
Scapula allata test
Spinal accessory neuritis
This nerve innervates the trapezius, who is responsible for the last 30° of glenohumeral adduction, therefore the active elevation will only be slightly limited, about -10°.
The complementary test here is, during active approximation of the scapulae, to pull the scapula laterally. Normally this is completely impossible ; in case of neuritis, because of the weak trapezius, we now can detect mobility.
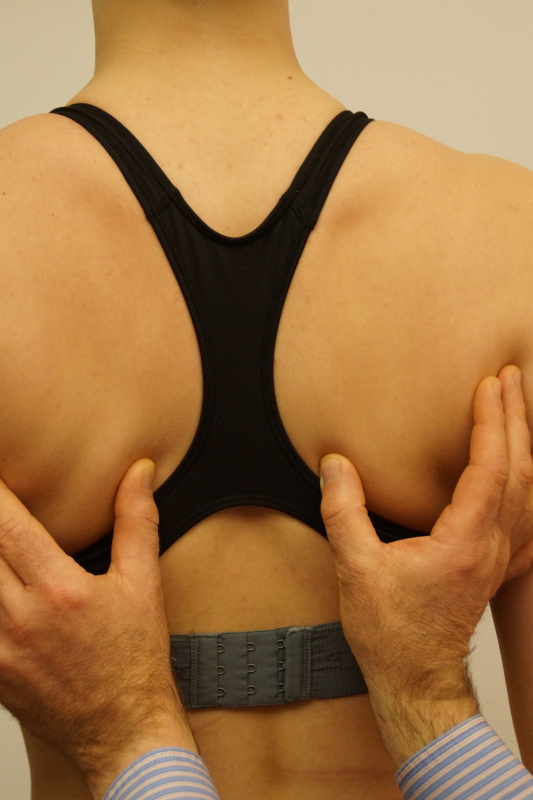 complementary test for spinal accessory neuritis
complementary test for spinal accessory neuritis
Treatment
1. If necessary specific medication
2. Passive end range shoulder mobilization in order to prevent a immobilisational arthritis
3. Electrotherapy to prevent further atrophy.
Note: the suprascapular mononeuritis is discussed in another chapter.
Fracture
Fracture of the spinous process C7 or T1 (“clay-shoveller’s fracture”)
Sudden spontaneous onset of a central lower cervical pain. We firstly suspect a cervical internal derangement, but the clinical examination discloses far too many positive signs for a derangement only : not only some active and passive neck movements are very painful (extension !) but also
- some resisted neck tests are also positive (extension)
- the resisted scapular elevation is painful and weak
- there is gross bilateral limitation on active arm elevation ; passive elevation is OK.
Fracture of the first rib
Sudden spontaneous onset of unilateral lower cervical pain or unilateral pain under scapula, or behind the clavicle .
It is more often the result of a stress fracture than a trauma. We expect healing in about 2 months.
Again, we don’t think of a cervical internal derangement because there are too many positive signs pointing in another direction : articular and muscular neck signs, a positive scapular test and a positive shoulder girdle test :
- neck : active and passive side flexion away from the pain are positive ; resisted side flexion towards the pain is positive (the scaleni muscles insert on the first rib)
- resisted scapular elevation positive
- unilateral limitation (less than in the previous case) on active, not passive, arm elevation.
Coracoclavicular ligaments
A lesion of the conoid - trapezoid ligaments can occur in certain sports such as squash and tennis and more specifcally during the phase before the smash.
It can also occur after a clavicula fracture.
The patient describes pain in the mid-clavicula area. Some end range passive shoulder- and scapula- movements are painful.
As an accessory test, the combination of passive lateral rotation and abdduction is painful.
Instability
The patient describes a combination of symptoms during activity : pain, weakness, and a subjective feeling of hypermobility. During arm elevation we could find a false positive painful arc .
It could be the result of a trauma : falling on the arm, straightened and in lateral rotation and abduction.
In order to confirm the diagnosis we need some accessory tests such as :
- Anterior apprehension test
- Posterior apprehension test
- (Load and shift maneuve).
It is the purpose to provoke the subjective feeling of instability during those tests.
 anterior apprehension test
anterior apprehension test
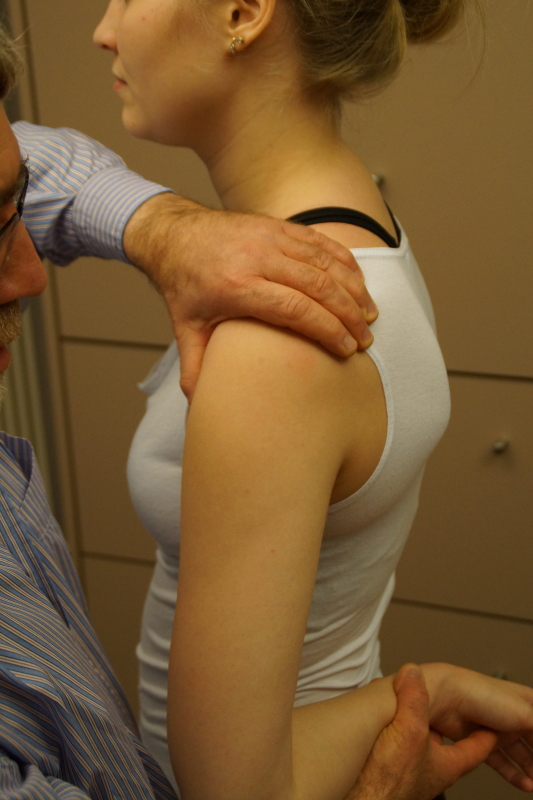 Posterior apprehension test
Posterior apprehension test
Snapping shoulder
The lig. transversale humerale is ruptured, causing some instability in the sulcus bicipitalis. The biceps “jumps” out the cranial part of the sulcus during certain activities, which could lead to an irritation of the tendon.
