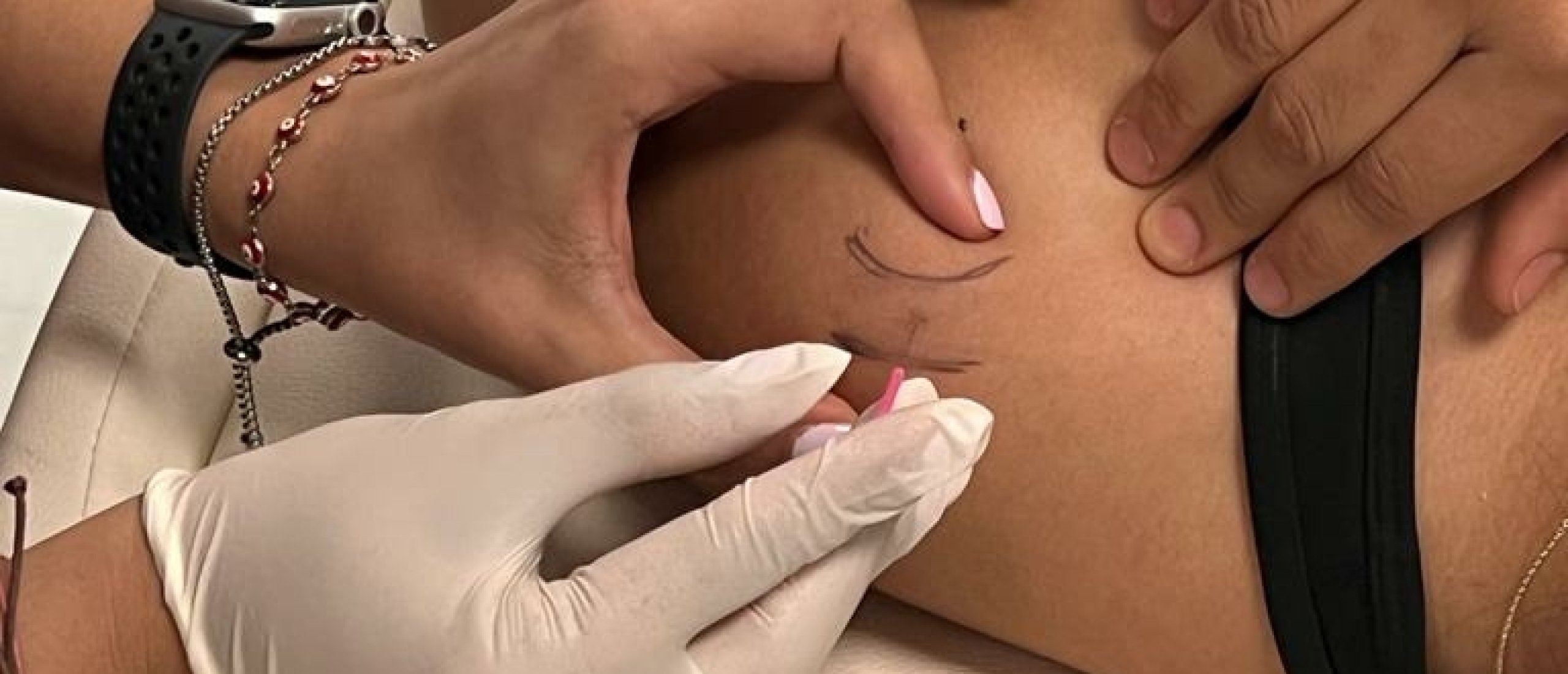
What is Percutaneous Micro Fenestration?
Text written by Mr. Pablo Romero, PT, ETGOM-GCI instructor, Latin-America
What is Percutaneous Micro Fenestration (PMF) of soft tissue lesions?
Micro: Refers to the size of the needle used to fenestrate. In case of echoguided tendon fenestration large caliber hypodermal infiltration needles are used, ranging from 18 G to 22 G (The most used 21 G: 0.8 mm in diameter).
In PMF on the other hand, low-caliber needles are used with an average diameter of 0.25 mm, similar to the needles used in acupuncture or in the dry needling techniques,. The length of the needle depends on the depth of the structure to be treated, varying from 25 - 30 mm to 40 - 50 mm.
Fenestration: This word comes from Latin: Fenestra, and means opening, hole. In orthopaedic medicine, the term fenestration refers to the action or effect of causing many holes or small holes in a specific soft tissue structure.
Percutaneous: It refers to penetrating through the skin.
Biological Effect
PMF has an irritating effect of mechanical origin, which is produced as a response of the injured tissue to the multiple microperforations by the needle puncture.
This controlled microinjury that occurs in the injured tissue will initially cause a worsening of symptoms again, inducing a local inflammatory process, which causes microbleeding and an increase in local blood flow, and thereby attracting different cells and mediators that will repair the tissues that have been fenestrated, triggering a natural inflammatory process.
This controlled inflammation is the first step in the wound healing process with the subsequent formation of granulation tissue, as well as the formation and remodeling of the extracellular matrix, thanks to the influx of granulocytes and, at a later stage, monocytes and macrophages.
Macrophages secrete various growth factors that in turn attract and activate fibroblasts. The fibroblasts deposit new collagen that eventually contracts causing the tissue to shorten.
With the tension generated in the new tissue, the collagen fibers progressively align in the direction of the tension exerted on them, which would ultimately increase the resistance of the tissue to traction.
Therefore the percutaneous micro fenestration technique is quite compatible with deep transverse friction massage techniques, as well as with different loading exercise strategies on soft tissue, which are essential.
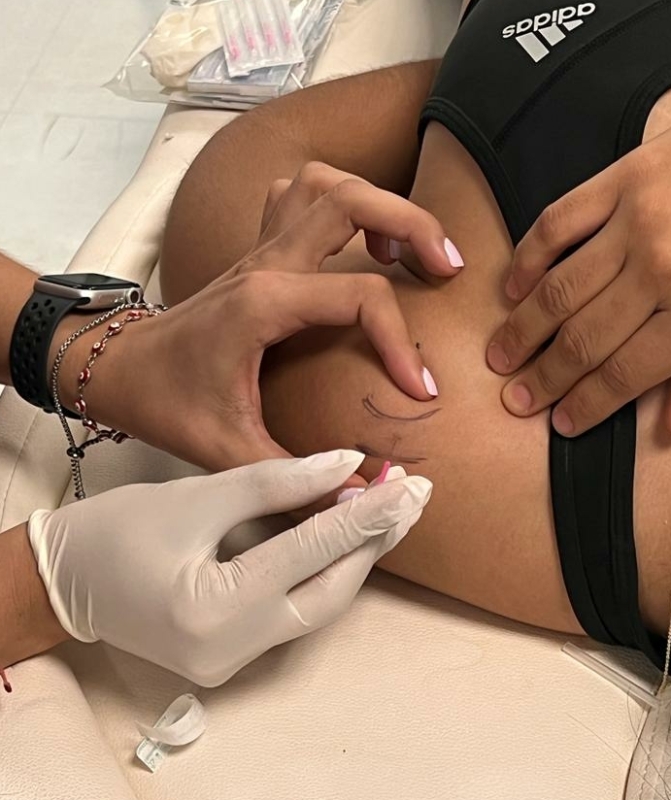 Percutaneous micro fenestration - supraspinatus tenoperiosteal aspect
Percutaneous micro fenestration - supraspinatus tenoperiosteal aspect
It is interesting to highlight the difference between PMF and corticosteroid infiltration:
- PMF has no anti-inflammatory effect. What it does is mechanically stimulate a local inflammatory reaction in a controlled way, to repair and “strengthen” tendons, muscles and ligaments.
- Corticosteroids, on the other hand, have a great anti-inflammatory effect but can have a negative effect, by weakening/damaging tendons, ligaments and joint cartilage.
- Although the initial effects of infiltration with corticosteroids are very good (in certain acute cases), by quickly relieving pain, the long-term effects could be unfavourable in some specific cases. Anyhow, in certain cases of tendinosis, the recurrence rate after corticosteroid infiltration is rather high.
Percutaneous micro fenestration Indications
PMF is indicated in chronic soft tissue injuries of the musculoskeletal system, such as tendinosis, some muscle and ligamentous lesions.
Pre-procedure Recommendations
Take care of proper desinfection first. And ask for the patient consent!
Before the PMF procedure, it is advisable to instruct the patient to avoid as much as possible the intake of nonsteroid anti-inflammatory drugs (2 weeks before and after the procedure).
Avoiding these medications, theoretically, can increase the chances of healing, since inflammation, growth factors and the healing cascade would not be altered.
The patient may also notice an increase in post-application pain, which will disappear approximately after 24-48 hours. (warn your patient about that).
We suggest to start a treatment session with the application of deep transverse friction massage (about 10’), then followed by the PMF. Thanks to the short term local analgetic effect of the friction massage, the PMF can be performed in more comfortable way for the patient.
 Percutaneous micro fenestration - correct palpation of the subscapularis
Percutaneous micro fenestration - correct palpation of the subscapularis
Technique and Procedure
First of all make sure you reach a relevant diagnosis and determine the exact spot where to apply the PMF.
A good understanding of palpatory anatomy is of course also crucial.
In case you wish to treat different locations, a different needle will be used for each entry point.
Once inserted superficially and directed, the needle will be inserted into the structure (if the lesion is tenoperiosteal then the needle is inserted until it makes contact with the bone), then the needle is slightly removed (without removing it outside the skin), and redirected sequentially fenestrating successively the entire surface.
Between 30 and 60 fenestrations will be carried out in a period of time ranging from 30 seconds to 1 minute, this will depend on 3 factors:
- The size and surface area of the lesion to be fenestrated.
- The degree of inflammation and exacerbation you want to obtain.
- The patient's tolerance to the pain generated by fenestration.
The needle is then left at the site of the lesion for 5 minutes, and then begins a new batch of fenestration just like the first (30 and 60 punctures).
Finally, leave the needle resting in place for 5 more minutes, to finally remove it and finish the treatment.
The total procedure takes about 10 - 12 minutes.
It is recommended to apply a next PMF session about 7 days after the first session.
Post-application considerations
Take into account the following post-application considerations of PMF:
- After tissue fenestration, the patient is asked to avoid anti-inflammatory drugs for 2 weeks so as not to interfere with the healing process.
- For similar reasons, avoid cryotherapy so as not to inhibit induced inflammation, which is the precursor of tissue healing.
- Avoid for 48 hours. physical activity that compromises and / or stresses the treated structure.
- Continue with specific physiokinetic treatment after 48 hours of PMF treatment. (i.e. deep transverse friction massage and different loading exercises)
Aseptic measures
- Use of sterile gloves before and during the procedure.
- Before the needle is inserted, clean the skin area with alcohol.
- When removing the needle, clean the area again with alcohol as subtle bleeding can be generated when removing the needle.
Contraindications
- Bleeding disorder; the use of anticoagulants
- Local infection, tumors
- Neuritis, capsulitis, bursitis
- Lacerations and/or skin wounds.
- Tear of more than 50% of the thickness of the tendon.
- Diabetes: insulin dependant.
- Rheumatoid arthritis, Gout, Psoriasis, Lupus.
- Psychoneurotic patient / needle phobia.
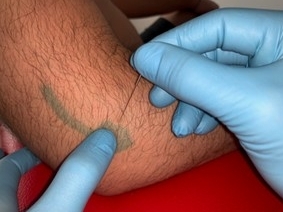 Percutaneous micro fenestration - tennis elbow type II
Percutaneous micro fenestration - tennis elbow type II
What's the difference with Dry Needling?
Dry needling is a technique for treating myofascial trigger points, it is not aggressive, the puncture is superficial and does not reach the periosteum, the objective is not to cause inflammation...,
in DN a clinical diagnosis is not required, prior analgesia is not required either because it is not aggressive and does not reach the bone either...
On the other hand, the objective of PMF is to cause a controlled micro-injury, therefore a precise orthopedic diagnosis, in addition to causing local inflammation, prior anesthesia is necessary (we achieved it with DTM).
In the treatment the tenoperiosteal union is fenestrated, therefore both the tendon and the underlying bone are punctured... in PMF guidance is also recommended by means of ultrasound.
The intervention guidelines in PMF are the same as those used by doctors in infiltrations for the different structures of the musculoskeletal system... in DN none of this prior knowledge is required (orthopedic clinical diagnosis, DTM, percutaneous access routes, interventional ultrasound) because it is just a myofascial trigger point treatment technique….
On writing this article I was also inspired by the article "Ultrasound-guided tendon fenestration" by Mary Chiavaras and Jon Jacobson; Semin Musculoskelet Radiol 2013;17:85-90
