- 7 things you need to know about a positive Straight Leg Raise - Lasègue
- Clinical interpretation of a positive straight leg raise or Lasègue
- So, let me guide you through some interesting SLR - Lasègue interpretations
- A painful arc on straight leg raise
- Importance of added neck flexion on straight leg raise
- The straight leg raise as a dural or as a root sign
- 6 different stages of a straight leg raise or Lasègue
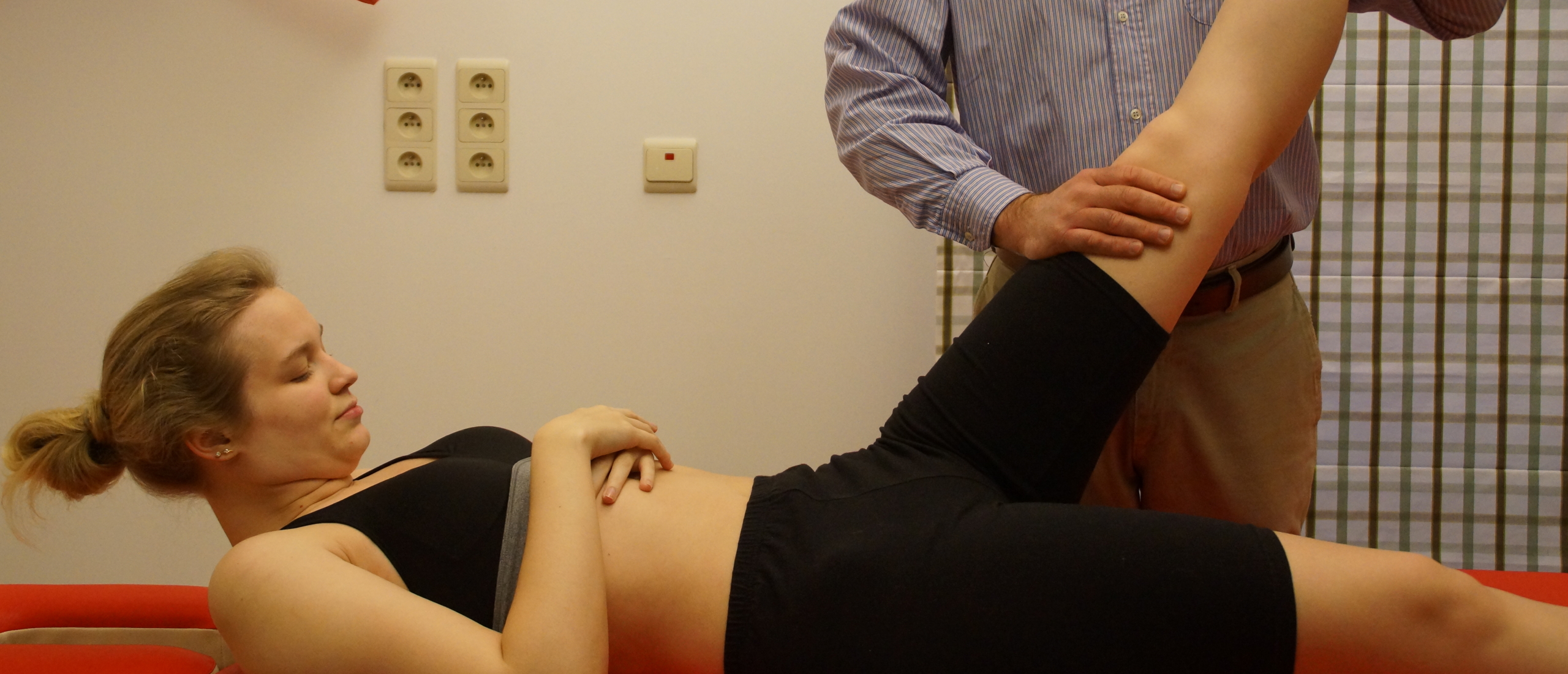
Straight Leg Raise or Lasègue test, how to interpret
7 things you need to know about a positive Straight Leg Raise - Lasègue
What exactly is a positive straight leg raise (SLR) or Lasègue? Keep in mind that a negative straight leg raise doesn't exclude a symptomatic lumbar disc protrusion or internal derangement. And, a positive SLR doesn't necessarily mean there's a sciatica.
Clinical interpretation of a positive straight leg raise or Lasègue
Important : this test is performed in a passive way and not in an active way, first on the painfree side, because we would like to find out which range of movement is normal for this particular patient.
Secondly, the patient can make a difference between a "normal" stretching of muscles-feeling and a different sort of pain, the pain which he actually complains of.
Many people perform the SLR or Lasègue test but apparantly they don't know exactly what the purpose is. "It's a nerve root test for sciatica" is the most common answer I receive.
In fact it is so much more. It all depends on which defintion of a positive SLR you are familiar with! Perform the test in a correct way and ask the right questions to your patient while doing the test. If you don't, you will surely miss a lot of positive tests.
Becoming successful in diagnosing and treating musculoskeletal disorders is more about using your brain instead of our "thinking fingers" :)
You would like to find out more about relevant clinical reasoning and therapy strategies? Why don't you join the Mastermind private training in orthopaedic medicine Cyriax. It surely will be an experience you'll never forget!
So, let me guide you through some interesting SLR - Lasègue interpretations
A painful arc on straight leg raise
A painful arc on straight leg raise is quite common, therefore on performing the passive movement we stop the movement whenever it is painful, we stay in this position, we ask the patient where he feels the symptoms and…we try to continue the movement !
Only in this way we can discover a painful arc. The diagnostic difference between e.g. -40° ROM of SLR versus a painful arc is significant (big limitation is most lileky caused by a big internal derangement ; a painful arc always points in the direction of a small lumbar internal derangement which is easily reducible).
Importance of added neck flexion on straight leg raise
We perform the SLR as far as we can, perhaps pain is produced (where exactly ?), then we add an accessory neck flexion. If the added neck flexion affects the pain (i.e. it can worsen the pain, abolish it or produce it (where ?), then this is a clear dural sign excluding the sacroiliac joints, the facet joints or muscles as the cause of the pain.
Remark : it is possible that accessory neck flexion, at the end of SLR, eases the pain instead of increasing it.
There probably is an anatomical explanation for this : in that case the protrusion probably lies medial to the nerve root. Neck flexion also exerts a cranial force on the dura, possibly resulting in less compression of the nerve root.
The straight leg raise as a dural or as a root sign
We consider the straight leg raise as being a dural sign if it provokes a dural pain (i.e. backache with or without radiation). Just like neck flexion stretches the dura cephally, SLR stretches it caudally. The dura also moves in an anterior direction on neck flexion and SLR.
Actually, we can state that any considerable limitation of dural mobility results in a positive SLR.
In an acute lumbago (big posterocentral internal derangement), the limitation of SLR is bilateral. Unilateral lumbago causes more a unilateral limitation/pain of SLR, or a limitation which is greater on one side. When the compression of the dura ceases, the range of movement becomes normal again.
Criterion as a dural sign
The SLR is a very useful criterion during a treatment session by manipulation/traction or by any other active methods. Interpreting the evolution of the limitation and/or pain during the SLR, we can easily interpret the gradual reduction of the internal derangement.
Example : suppose a patient has backache and 20° limitation of SLR. We start manipulation (if indicated) using the SLR as a test-retest criterion inbetween the manoeuvres. After a first manipulation, the test shows 10° limitation is left. After the next maneouvre, SLR becomes negative, allthough there is no full reduction yet ; some movements in standing may still be painful. We continue manipulation, but from now on the positive movements in standing become our new criterion.
The SLR clearly shows us whether the treatment we deliver is clinically effective.
Criterion as a root sign
Example : a three week old sciatica with 30° limitation of SLR. The treatment is ,e.g. daily continous mechanical traction. The SLR is tested before every traction session.
At the end of the first week, only 10° limitation remains. In the week-end, the patient makes an excursion with his family, sits in his car for hours and hours, and when he comes back after the week-end he again has 30° limitation of SLR. What does that mean ? Indeed, it is worse again, but not worse than the beginning ; we can still continue with our treatment. If SLR would be e.g. 60° limited, then probably we would have to change the treatment strategy.
6 different stages of a straight leg raise or Lasègue
- Negative : a minor disc protrusion is still possible.
- Painful, not limited : the protrusion cannot be large and must be rather small.
- Painful arc : this is a wonderfull dural sign point in the direction of a small protrusion, with dura or nerve root catching against it and sliding over it.
- Painful, limited, without neurological deficit : a somewhat larger protrusion, interfering with mobility, not with conduction.
- Painful, limited, with neurological deficit : severe compression, not only of the dural sleeve about the nerve root, but also of the parenchyma. Both mobility and conduction are disturbed.
- Negative with neurological deficit. The patient has had sciatica for some time. Now the pain gets even worse for minutes or hours or days, after which rather suddenly it disappears completely and SLR becomes negative again. This is an ischaemic root atrophy : the protrusion is maximal, the compression is so severe that the nerve root has become ischaemic. Stretching it causes no protective reflex anymore and SLR ceases to hurt. There is motor and sensory deficit, possibly with loss of knee or ankle jerk. The patient has become symptomatically better (no more pain) but anatomically worse.
Small internal derangement : think of one the first three options.
Bigger internal derangement : think of options 4-6.
Adherent nerve root
A past lumbar internal derangement causing an episode of sciatica has resolved but the repair process has left some tethering or adherence that now inhibits full movement of the nerve root/dural complex. Flexion in standing is limited and the patients feels end-range pain in the back or the leg (this is the only dysfunction syndrome that can cause peripheral pain ; all others cause spinal pain only).
The treatment of an adherent nerve root will consist of an intense stretching program.
Keep one important message in mind : one single positive test has no clinical meaning at all ; focus on the complete image : history, inspection and a cluster of positive and negative tests. For more detailed analysis and recent scientific background of the clinical images described above, I refer to the ETGOM training programs in Modern Orthopaedic Medicine Cyriax and to our publications.
