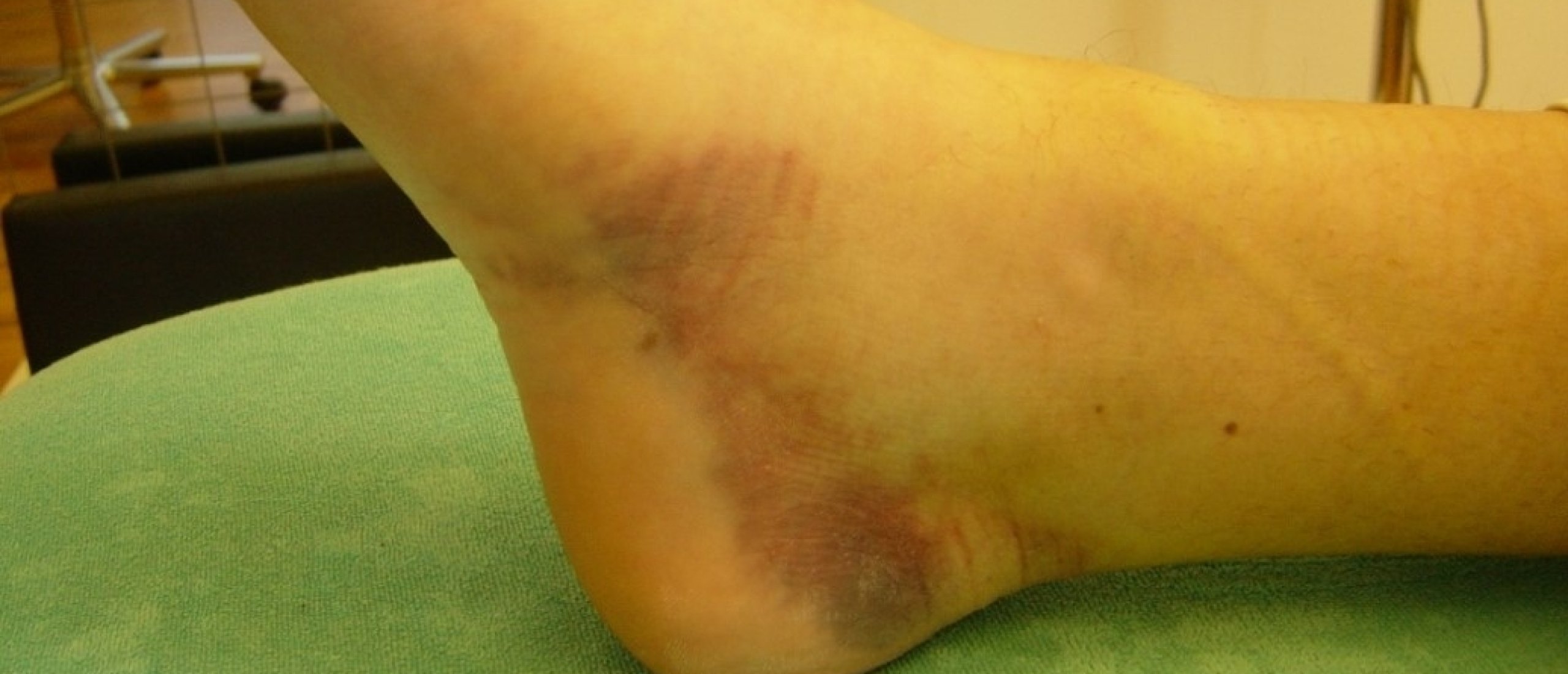
Ankle sprain differential diagnosis
Sprained ankle: ligamentous, articular or tendinous lesion, how to differentiate?
Was there an inversion or eversion trauma? A sprained ankle mostly is the result of an inversion trauma.
But the question is, what's the problem? Is there a ligamentous sprain, or a tendinous lesion, or even the combination of both? Perhaps there also might be an articular lesion (or even a joint malpositioning).
Since in acute cases the ankle mostly is swollen, it is really very important to manage well the technical details of your functional examination. This examination procedure probably is the more difficult one in the field of orthopaedic medicine.
Practice makes perfect! What's the next step to become an expert in orthopaedic medicine Cyriax? The Mastermind private training in orthopaedic medicine Cyriax offers you a series of useful solutions to improve your clinical reasoning and therapy skills.
Discover more about the ankle in following webinar recording.
A patient who sprained his ankle usually describes a varus trauma. In rare occasions there will be a valgus trauma with pain at the medial or postero-medial side of the ankle.
Varus ankle sprain or inversion trauma
An inversion trauma is a combined movement. Depending on which movement was dominant, the lesion can
be different :
1. plantiflexion at the ankle provokes stress on
- anterior talofibular ligament, tibiotalar ligament and extensor tendons
2. varus at the talocalcanean joint stresses the
- peroneal tendons
- calcaneofibular ligament
3. adduction and medial rotation at the mid-tarsal joints put strain on the
- calcaneocuboid ligament.
Usually a combined ligamentous lesion is found. The combination of a ligamentous and a tendinous lesion seems to be less frequent.
In the “hitparade” following lesions are most frequent :
- Anterior talofibular ligament, fibular insertion
- Calcaneofibular ligament, fibular insertion
- Anterior talofibular ligament, talar insertion
- Calcaneocuboid ligament
--> Those represent the absolute “top four”, followed by
- Peroneal tendons
- Posterior talofibular ligament
- Extensor tendons
(Exceptionally : cubonavicular lig., cubometatarsal IV-V lig.)
Ankle sprain treatment
Purely ligamentous sprain
Acute stage (24 hours)
The PRICE principle (Protection, Rest, Ice, Compression, Elevation) only has an advantage in very acute cases and can shorten the recovery period, only if the immobilization doesn’t last longer than 3 days.
Early mobilization is the key to the restoration of function in all grades of ligamentous sprain. There will be a better overall result and faster rate of recovery
Functional treatment is the treatment of choice for the acute sprained ankle.
We perform cross friction massage, in a progressive way and moderate active mobilisation.
The first week daily treatment followed by 3x/week as from the second week.
Make sure to build in the transverse friction massage in a progressive way i.e. maximum a few minutes to start with and at the end of the first week we reach the normal portion of about 15 minutes.
Subacute stage
Same strategy as for the acute stage, but as soon as possible we need to add proprioceptive exercise.
Addition of proprioceptive training demonstrates a significant reduction in subjective instability and functional outcomes.
We expect the patient to be significantly better by the end of the first week ; in that case we proceed with the treatment. If, however, during the first days there is no improvement at all, further examination (medical imaging) should be considered.
Beware of following suspicious signs :
- clear pain on subtalar valgus
- compression # malleolus ?
- pain and weakness on R eversion
- fracture base meta V ?
- practically no pain on testing
- perhaps total rupture ?
- Marked bony tenderness to palpation
- Fracture meta V ?
Chronic stage
We hear the typical history of a chronic lesion : there was a trauma, at least 6 weeks ago, followed by immobilization only or the absence of treatment. Activities of daily life are symptomfree ; only when the patient does more intense acitvity, he feels it is not optimal. There is some pain, possibly some local swelling, for a few days.
Treatment : manipulative rupture of the adhesions after a preliminary DTM. Followed by some sessions of DTM and proprioceptive exercise.
Sprain with a tendinous lesion
We have to perform a “double” treatment, DTM for the ligament and the tendon.
Again with active mobilization and proprioceptive exercise.
Recurrent varus sprain
Most likely this is the result of a delayed contraction of the peronei, which is treated by a intensive proprioceptive training.
Valgus ankle sprain or eversion trauma
First we need to check whether there is a valgus deformity of the heel with abduction of the forefoot. In that case a medial support is advisable.
Furthermore, the deltoid ligament can be treated with an infiltration of triamcinolone (for a reason unknown to us, the deltoid ligament does not respond very well to DTM). An occasional lesion of the tibialis posterior responds well to DTM.
