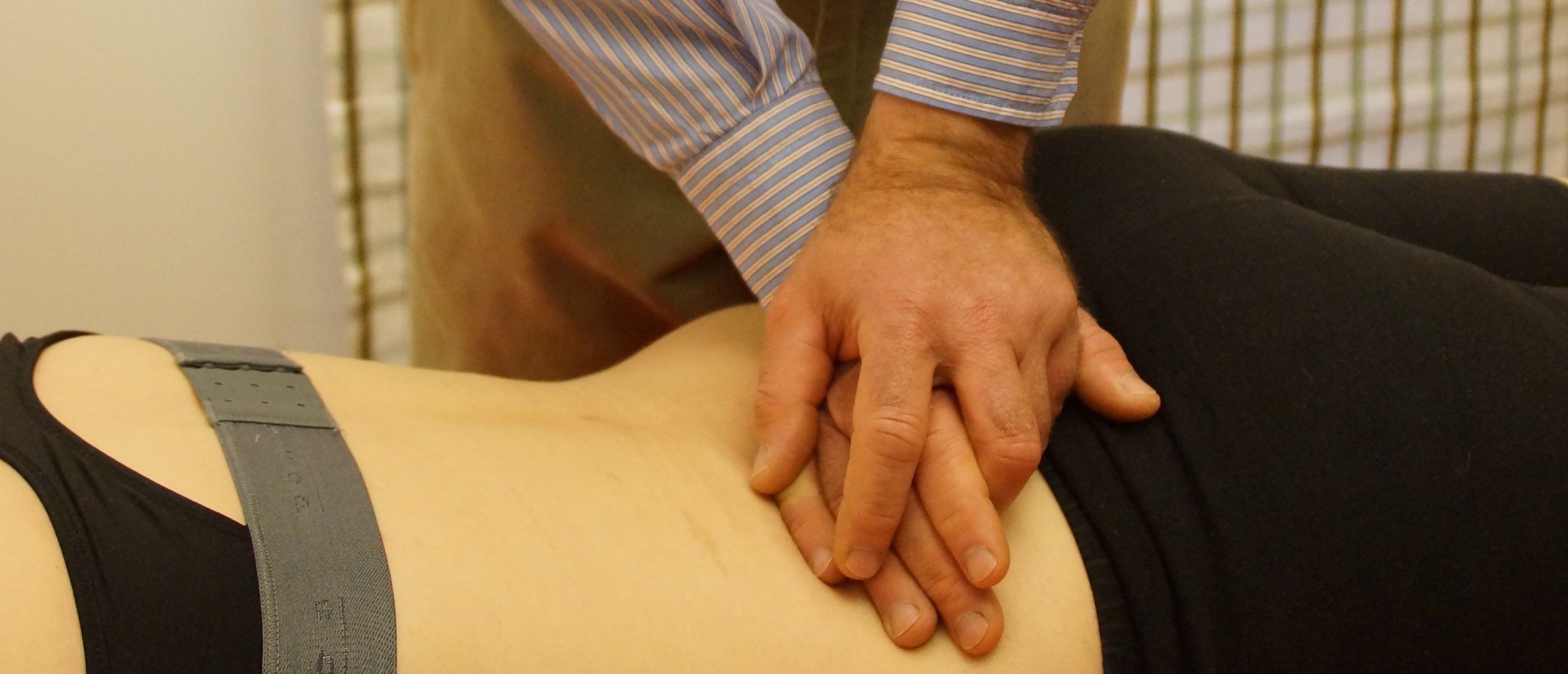
Lumbar spine functional examination
Which tests are useful when you examine the lumbar spine?
When it comes to the fuctional examination of the lumbar spine, numerous tests and interpretations are described in literature.
I sincerely believe It doesn't make sense to "over-test" the patient. In fact, many manual test procedures (e.g. in relation to segmental "hyper-hypo mobility") seem to have a very poor validity, so let's focus on those tests or clusters of tests that really help me to reach a more useful diagnosis.
Keep in mind that the value of one single positive test is zero. We always look for specific clusters of positive and negative tests so that we can interpret the clinical image in a more reliable way.
It is important to look at the "package" i.e. data from the history, the inspection and the functional examination ; in some cases data from medical imaging could be useful too.
Performing those functional examination tests is not "rocket science" ; it's in fact very easy! You don't need 5 years of university training to manage that :)
The challenge however is how to analyze the test results! And this requires some study and training. How can we interpret the clinical pattern, what does it mean, which are the diagnostic and therapeutic consequences?
The quality of your interpretation will have a direct effect on the efficiency of your treatment strategy!
That's exactly what you will learn during the Mastermind private training in modern orthopaedic medicine Cyriax. Focus on what really matters, without any "artificial hypercomplication"!
So, let's have a look at the film
There's so much more to discover...
Lumbar spine assessment - inspection
The lumbar spine assessment also includes tests for the hip and the sacroiliac joints, since those joints can refer pain in the back, the leg or the gluteal area. Should such a test be positive, the whole hip or sacroiliac examination has to be added.
We look for :
- bony signs
- articular sign
- dural signs
- root signs (mobility, conduction)
- (cord signs).
In fact, the inspection starts as soon as the patient comes in : how does he walk, how does he sit during the history-taking, what is his expression ?
A patient with an acute lumbago may prefer to stand instead of sit during the history-taking. A patient may perform trunk flexion movements in sitting without any problem at all (e.g. for taking something from her handbag) and a few minutes later, on examination, prove unable to bend forward.
Inspection reveals such a contradiction.
It is a good idea to make the patient undress in view of the therapist and not hidden behind a curtain in some cabin. We could, in this case, immediately see which movements seem painful, and which movements should be corrected to avoid recurrences.
It is even more important to see how the patients dresses again ; we should give him to the point prophylactic advice (see further).
After having taken a history, the patient stands in front of a mirror and we stand behind the undressed patient and look particularly for :
Bony signs
>>> An angular kyphos, although it can be innocuous (erosion of two adjacent discs), could indicate a vertebral pathology (a fracture due to osteoporosis, metastases, or local osteitis deformans). Medical imaging is needed to elucidate the nature of the deformity,before we would consider manipulation.
>>> The rounded kyphosis of Scheuermann’s disease (disc erosion at various levels), on the contrary, is not dangerous.
>>> A shelf can be palpated in standing, by gliding downwards with our fingertips over the spinous processes. It indicates the presence of spondylolisthesis ; it does not necessarily indicate that the actual symptoms are also caused by the spondylolisthesis (interpret the history!).
Leg length difference
How to discover a leg length difference without medical imaging .
Have a look at five variables, when all of them point in the same direction, then there is leg length difference :
- Level cristae iliacae
- Level SIPS
- Level SIAS
- Level caudal aspect glutei
- Measure distance from SIAS --> caudal medial malleolus
If a difference has been found, then most likely there is no relation with the patient’s actual symptoms.
One can “correct” the difference by putting boards under the shorter leg. If this would have a favourable effect on the symptoms during the test movement in standing, then a raised heel is recommended. A difference of less than 1 cm is considered irrelevant.
It is also useful to observe the equal distribution of body weight over both feet. A patient with a posterolateral disc protrusion or with a neoplasm of the ilium can be seen, on the affected side, to put only the toes on the ground.
Deviation – antalgic posture
Flexion deviation ?
A patient is blocked in flexion, extension is very limited and painful : most likely this is the result of an acute posterocentral internal derangement.
If he deviates from the hips and not from the lumbar spine, then a hip problem is suspected.
A lateral deviation can be relevant or irrelevant.
A lateral deviation with a rotation component is due to scoliosis and therefore mostly irrelevant (except for the “formula 1-scoliosis”), because it is unconnected with the present symptoms.
How to discover a scoliosis : on trunk flexion, one side of the back is flattened and the other side is curved.
A lateral deviation without rotation component is relevant : it is an antalgic posture and therefore related to the patient’s symptoms. (An exception, extremely rare, is a hemivertebra.)
We will discuss six types of lateral deviation, all related to a symptomatic internal derangement :
- Away from the painful side
The protrusion lies “at the shoulder” of the nerve root
2. Towards the painful side
The protrusion lies “at the axilla” of the nerve root. This is slightly more frequent than the previous case.
3. Alternating deviation
The patient is deviated, say, to the right ; after trunk flexion he now has a left deviation. This is a rather small protrusion, exactly on the midline ; the dura mater tries to escape compression to the left or to the right.
4. Deviation in standing, disappearing in full flexion - Deviation in full flexion, not in normal standing
The general significance of a lateral shift / deviation is that the protrusion is larger than without a deviation, i.e. that more treatment sessions will be required to obtain reduction. If the patient does not lose his deviation in any posture, then the protrusion is larger than in the last two cases, where he has a deviation in one position and not in another.
5. Momentary deviation (“painful arc”)
The patient has no deviation in standing, he does a flexion and somewhere at midrange he shows a momentary lateral deviation, at the end of the flexion movement, there is no more deviation. Of all types of deviation, this is the most favourable in terms of reduction chances by manipulation or traction.
A large lateral deviation / shift is much more often due to an L4- than to an L5-protrusion. Because of the shape of the bones and the presence of the iliolumbar ligaments, the L4-disc has a greater lateral mobility than the L5-one.
In all types of deviation, described above, we see a lumbar correction for a lumbar problem : the shoulders remain at the same height.
6. Deviation of the"hysterical" patient
This deviation is quite different : we see a thoracic, or even cervical, correction for a “lumbar” problem, with one shoulder kept up.
Lumbar spine assessment - tests in standing
>>> What does the patient feel at this moment ?
Is there any pain at rest and where is it felt ? We have to interpret whether the test movements have any influence or not on this pain.
>>> Active lumbar movements
The patient performs four active lumbar movements and we ask him whether any of them bring on or alter his pain.
Instead of asking “does that hurt ?”, it is more objective to ask “is there any change ?”.
Possible answers are :
- No change, incomparison to the status at rest
- More pain
- A new pain is produced, possibly somewhere else
>>> Always check the localization of the symptoms.
The movements are : extension, side flexion and flexion.
At the end of the flexion we ask the patient to add a neck flexion as a complementary dural stretch : there could be more pain or even less pain on this extra test, a typical dural sign.
We assess pain (where and when) and range of movement. Because of the possibility of a painful arc, it is important that the patient does not stop at the first appearance of pain ; we should check whether he can continue the movement beyond this pain or not.
As a therapist it is imperative to stand behind the patient, otherwise we can miss the appearance of a lateral shift /deviation on flexion.
The last test in standing is the unilateral rising on tiptoe. This is a motor test for the S1/S2-nerve roots ; we assess muscle strength.
Tests in standing : clinical interpretation
The full and partial articular pattern
At this stage in the examination we already make a distinction : did we see the clinical pattern of an arthritis or that of e.g. an internal derangement, in other words did we find a full articular pattern (= capsular pattern) or a partial articular pattern (= non-capsular pattern) ?
The full articular pattern is an equal limitation of extension and both side flexions, with flexion being the best movement.
If we see this pattern in a 70 years old patient, the cause is probably osteoarthrosis ; if we see it in a 30 years old patient, something else is going on, e.g. ankylosing spondylitis.
Any other combination is the partial articular pattern. This is what we expect in an internal derangement.
The combination of a partial articular pattern and a painful arc on flexion is very significant and is interpreted as follows :
- the symptoms are not psychogenic
- The lesion must be an internal derangement
- It is a favourable sign for reduction in general and for manipulation in particular, because a painful arc points in the direction of a slight, easy reducible protrusion.
Red – orange flags
1. If an articular movement produces or worsens symptoms in the leg instead of the back, then this is rather unfavourable. This is a kind of peripheralisation ; reduction of the internal derangement by conservative therapy will be more difficult
2. Side flexion towards the painful side increases the backache.
In both previous cases, we suspect (empirical experience) that continuous mechanical traction is more efficient than manipulation.
Extension and both side flexions are the real articular movements ; flexion (with added neck flexion) is mainly a stretch of the dura mater and the nerve roots L4/L5/S1/S2.
Trunk flexion and straight-leg raise / Lasègue are in fact the same test, with the difference that the former is done under compression.
Tests have no influence on the pain ?
It is possible that the tests are too “light” in order to discover a particular pathology, therefore it is imperative to try to influence the symptoms by increasing the intensity of the test or by repeating the test.
This will provide valuable differential diagnostic information e.g. we can then discover a dysfunction syndrome (see further).
Lumbar spine assessment - tests in supine lying
Sacroiliac distraction test
We bear in mind that the sacroiliac joint is a unilateral structure and, therefore, can only cause unilateral pain. Hence, not every pain on this test will be interpreted as a positive answer. The correct approach is as follows :
1. First question : where did you feel that ?
>>> “where your hands lie” : test negative, proceed to the next test.
>>> “In the back” --> next question.
2. In the middle or to one side ?
>>> “in the middle” --> test negative, since a unilateral structure cannot cause pain on the midline.
>>> “Left” or “right” --> repeat the test in the second, more supported and intensive, version.
3. The test is repeated in a slightly more forceful way, but this time with the forearm behind the back stabilizing the lumbar spine, thus increasing the lordosis :
>>> “better” --> the test is negative, since apparently there is a direction relation with the optimalisation of the lordosis.
>>> The patient feels unilateral pain in the buttock : positive test, continue with the accessory SI-examination.
Straight-leg raise / Lasègue (+ neck flexion ?)
From now on, we perform all tests bilaterally, the good side first.
The straight leg raise test is done in a passive way and we assess pain and range of movement ; then a neck flexion is added and its effect assessed. Make sure you reach the real end range ! A painful arc can be found.
Hip : passive flexion and rotations
We assess pain, range of movement and end-feel (elastic).
Radicular tests
Motor conduction
- iliopsoas L2-L3
- tibialis anterior L4
- extensor hallucis longus L4-L5
- peronei L5-S1
Sensory conduction : we look for sensory deficit in the distal part of the dermatomes. We test both sides simultaneously :
- distal part of anterior thigh L2
- distal part of anterior leg L3
- big toe L4
- inner side of foot, toes 1-2-3 L5
- outer side of foot, toes 4-5 S1
- plantar aspect of heel S2
Knee jerk L3
Plantar reflex / Babinski
We test the plantar reflex by means of a “half-moon” movement. Flexion of the toes is a negative answer. Extension of the big toe and spreading of the other toes suggest spinal cord compression with, as a consequence, a bar for active treatment ; further examination is needed.
Tests in supine lying : clinical interpretation
Straight-leg raise / Lasègue
>>> First on the painfree side
Firstly we have to find out which range of movement is normal for this particular patient. Secondly, the patient needs to distinguish between a “normal” (painful) stretching of muscles and his actual symptoms.
>>> A painful arc
Since a painful arc at SLR is not uncommon, we should not abandon the test as soon as pain is provoked. The moment we provoke pain, ask for the localization of the pain and then continue with the movement, possibly provoking a painful arc. A painful arc points in the direction of a small and easy reducible internal derangement.
>>> Neck flexion
If the added neck flexion affects the pain, then this is a clear dural test : we exclude the sacroiliac joint, the facet joints or the hamstrings as the cause of the pain.
We can expect three possible reactions :
- No influence on the pain
- More pain (in the back, gluteal area or leg)
- Less pain
>>> The SLR is not only a root test but also a dural test.
Just like neck flexion stretches the dura upwards, SLR stretches it downwards. Actually, we can state that any considerable limitation of dural mobility results in a limited or painful SLR.
The limitation is mostly bilateral if the pain in the back is central/bilateral, e.g. in an acute lumbago, a large central protrusion compresses the dura mater resulting in clear dural signs.
A unilateral internal derangement can cause more a unilateral limitation of SLR, or a limitation which is more prominent on one side. When the compression of the dura ceases, the range of movement becomes normal again.
The SLR is a very useful criterion during a treatment session by e.g. manipulation. We can easily follow the gradual reduction of the disc protrusion by means of the evolution of the SLR.
Example 1 : a patient with backache and 30° limitation of SLR. We start manipulation using SLR as a control test criterion inbetween the manoeuvres. After a first manipulation, the test shows about 10° limitation. After the next manipulation, SLR becomes negative, although there is no full reduction yet. Some movements in standing may still be painful. We continue our manipulative strategy (see further), but from now on the positive movements in standing become our new control test criterion.
Example 2 : a three week old sciatica with 30° limitation of SLR. The treatment is e.g. daily traction ; every day, the SLR is tested before traction begins. At the end of the first week, only 10° limitation remains. In the week-end, the patient makes an excursion with his family, sits in his car for hours, and when he comes back on monday he has again 30° limitation of SLR.
Now we do not continue traction : we see that the situation is worse again, but we do not know yet how much worse. So, we do the complete examination, and if we do not find any neurological deficit, we go on with traction.
If, however, we find neurological deficit, we know that the protrusion has become too large and therefore irreducible and we think of e.g. epidural local anaesthesia as the next step in the treatment.
Conduction – Palsy
When a disc protrusion compresses a nerve root, we can find a monoradicular or a biradicular deficit or even half a palsy (only motor or only sensory).
The interpretation of a palsy is twofold :
- first, a neurological deficit means that the protrusion has become irreducible, i.e. that manipulation, traction or exercises are no longer indicated. Epidural local anaesthesia is the next step in the treatment.
- Second, if we know which root is compressed, maybe we also know which disc causes the compression :
>>> L4-root : compression by the L4-disc
>>> S1-root : L5-disc
>>> L5-root : there could be compression either from an L4- or an L5-disc.
About the localization of nerve root compression by a disc protrusion : most cases occur at
L4- or L5-level, and the frequency decreases higher up :
L3 : 5 %
L2 : 1/1.000
L1 : 1/10.000.
Red flags
- An L2-palsy (1/1.000 !) : serious pathology is much more likely (neuroma, metastases)
- The wrong combination, simultaneous compression of two roots :
>>> L4- and L5-roots : can be an L4-disc
>>> L5- and S1-roots : can be an L5-disc
>>> But L3- and L4-roots : cannot be compressed by one disc protrusion only
- Any combination of more than two roots : a disc protrusion is unlikely
- A compression to two non-adjacent nerve roots is also suspicious
- The same applies for bilateral or extreme weakness : serious pathology is suspected.
Lumbar spine assessment - tests in prone lying
Ankle jerk L5-S1-(S2)
Radicular tests (motor conduction)
Hamstrings S1-S2
Quadriceps L3
Passive knee flexion L3
This is a stretch of the L3-nerve root via the femoral nerve.
Contraction of the gluteal muscles S1-S2
Wasting of the muscles, found on palpation during contraction, is interpreted as a motor
deficit.
Palpation and extension pressure on the spinous processes
First we perform a palpation along the spinous processes for discovering bony or ligamentous abnormality. Then an extension pressure is applied from L1 to S1, asking the patient at which level his symptoms are best reproduced.
Execution : we apply the middle of the fifth metacarpal bone onto the spinous process, the hand is held almost flat and reinforced with the other hand. Both arms are extended, our slightly spread thighs lean against the couch, we use part of our body weight to take up the slack and with more body weight we provoke each segment. We assess pain and end-feel (normally elastic). We don’t assess any so-called hyper- or hypomobilities since this is highly irrelevant.
Some considerations :
>>> In repeated studies of manual therapists’ palpatory skills in the spine, poor intertester reliability has consistently been shown
>>> Palpation for tenderness can be very misleading due to primary and secondary hyperalgesia
>>> Inter-tester reliability of palpation techniques in the lumbar spine is consistently poor
>>> Studies that have used experienced clinicians have not shown better results than studies involving student physical clinicians or chiropractors. The large amount of variability in spinal stiffness values between subjects, or at different levels within the one subject, makes the determination of areas of abnormally increased stiffness difficult. Increased stiffness may in fact be a normal variant and bear no relationship to the patient’s presenting symptoms.
Tests in prone lying : clinical interpretation
Ankle jerk
A lost ankle jerk will not recuperate in 50 % of all cases. This means in practice that, if this were the only neurological deficit found in a new sciatica, it can be disregarded since most likely it is unrelated to the new sciatica, but the result of a previous sciatica.
Passive knee flexion
A test for the mobility of the L3-nerve root, through the femoral nerve. We do not really expect a limited range, but rather pain in the lumbar area or at the front of the thigh.
Complementary tests
The basic examination, described above, is used when we have heard a perfectly normal history, devoid of inherent unlikelihoods or possible alarm-bells. However, a complementary examination is needed in the following cases :
- when a muscular lesion is suspected (depends upon the history).
- Whenever an injury is mentioned (e.g. possibility of a fractured transverse process).
- When a psychogenic origin of the symptoms has not yet been excluded (we would then expect markedly positive resisted tests in comparison to some other tests).
- When we suspect a dysfunction syndrome (see further).
The most important complementary test is performing the basic test movements in a repeated way and interpret the effect of repeated movements (see further). This will be necessary to make the distinction between an internal derangement and a dysfunction syndrome.
In standing : both side flexions against resistance
In case of a fracture of a transverse process, this test will be positive.
Prone lying, A-P-R extension
In case of a real muscle lesion, the active and the resisted version will be clearly painful and the passive version will be negative.
